Our multidisciplinary team is made up of clinical oncologists, therapeutic and diagnostic radiographers, physicists, engineers, nurses, health play specialists, mould room technicians and Macmillan support workers. Together, we provide highly specialised patient-centred treatment and care, using the latest equipment and proton beam therapy techniques.
We are also committed to continuous learning and improvement, and have strong academic links with the UCL Cancer Institute and the UCL Medical Physics and Biomedical Engineering Faculty.
Therapeutic radiography students work in the department alongside the radiographers; they are under supervision at all times.
Consultant clinical oncologists are doctors who supervise your treatment and care. They use both proton beam therapy and chemotherapy, along with a range of other treatments as part of a patient's treatment plan. The consultant leads a team of doctors.

Consultant radiographers are therapeutic radiographers. They have undertaken in depth training in the specific anatomical area they specialise in such as breast cancers. They use and plan a patients proton beam therapy in conjunction with a range of other treatments a patient may be given as part of a patients overall treatment plan.
Specialist registrars and clinical fellows are doctors who specialise in Proton Beam Therapy (PBT), undertaking both clinical and research work. They use both PBT and chemotherapy, along with a range of other treatments, to create a patient's treatment plan.
Therapeutic radiographers
Therapeutic radiographers are allied health professionals (AHPs) who have undergone specific training to be able to plan and deliver radiotherapy and proton beam therapy, along with the holistic care of patients throughout their treatment.
Diagnostic radiographers
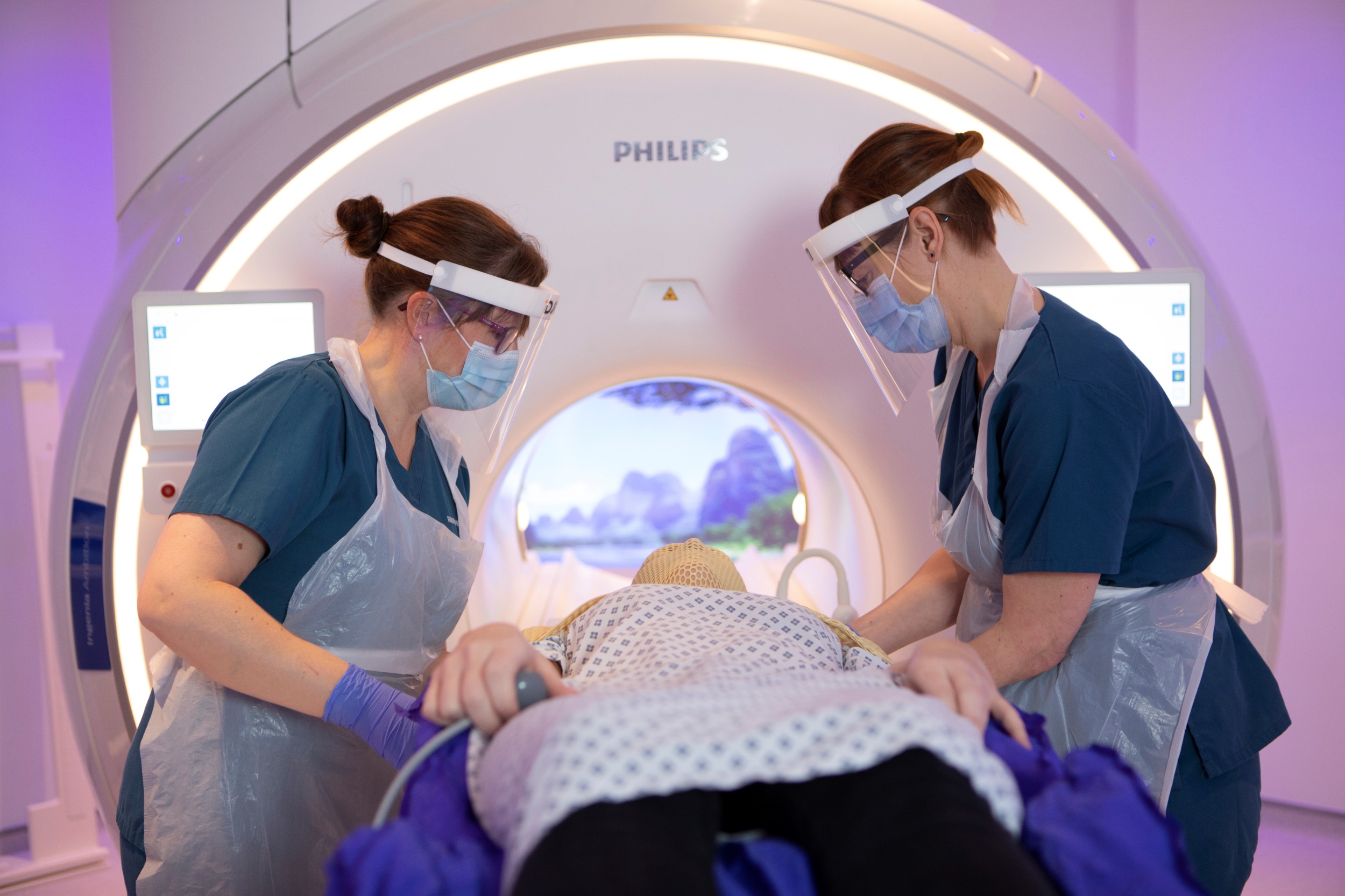
Diagnostic radiographers are AHPs who have undergone specific training to be able to work in areas including CT, MRI, ultrasound, fluoroscopy, angiography, nuclear medicine and mammography. In the Proton Beam Therapy department they use both CT and MRI to help plan a patient’s treatment.
Specialist radiographers
Specialist radiographers have undertaken additional training in the specific anatomical area they specialise in such as paediatric, sarcoma, head and neck, and neuro-oncology. These radiographers act as key workers whilst patients are away from their local hospitals. They ensure the radiotherapy treatment pathway and daily treatment is tailored to a person’s needs. They work very closely with other medical professionals to support and guide patients through their treatment.
Radiotherapy nurses work alongside as part of the larger multidisciplinary team, to review radiotherapy side effects and provide additional care for patients throughout their treatment.
The general anaesthetic team works closely alongside other staff, for patients who require a general anaesthetic for their procedures. The team consists of consultants, nurses and operating department practitioners.

Radiotherapy physicists and dosimetrists work as part of the larger multidisciplinary team to plan radiotherapy treatments. They are responsible for ensuring the quality assurance of radiotherapy equipment and the development of new technologies and techniques.
Radiotherapy engineers are specially trained staff responsible for preventative maintenance and the quality assurance of radiotherapy equipment.
Mould room technicians work alongside as part of the larger multidisciplinary team to create the individualised equipment required for radiotherapy treatments, and play a major role in the planning of some patients' treatment.

Health play specialists are specially trained staff to use play and other specialist techniques, to help children understand and prepare for differing radiotherapy procedures.

Our support workers provide emotional support and practical advice to help meet the holistic needs of our patients. They help patients gain access to health and social care by signposting them to support and advice services relevant to their needs.

Our administration and clerical team coordinate the booking of your treatment and any additional requirements you may have such as accommodation and transport. You may also see them on our reception desks and in our waiting areas each day to welcome you to the service.

Our speech and language therapists help children, young adults, and adults who are experiencing difficulty swallowing or speaking while undergoing proton beam therapy treatment. They work as part of a multi-disciplinary team to optimise a patients abilities, reduce side effects and provide rehabilitation.
They may also refer you to local Speech and Language Therapy Services once you’ve finished proton beam therapy if you need further support.
Physiotherapists help children, teenagers, young adults, and adults whom may be experiencing physical difficulties as a consequence of living with cancer, or undergoing cancer treatment. They also support patients to be physically active during their treatment.
Our physiotherapist can refer you to your local physiotherapy services once you’ve finished proton beam therapy if you require further support.
Our occupational therapists help children, teenagers, young adults and adults to maintain independence with daily activities throughout their treatment.
This is done by looking at what tasks a patient wants or needs to do, what makes this difficult for them and providing interventions to enable our patients to be able to do these activities.
Our dietitians work with children, teenagers, young adults and adults providing individualised plans which aim to:
- Meet nutritional requirements throughout treatment
- Avoid changes in body composition during treatment
- Manage side effects which may impact nutritional intake
- Optimise treatment outcomes
- Support ongoing recovery








